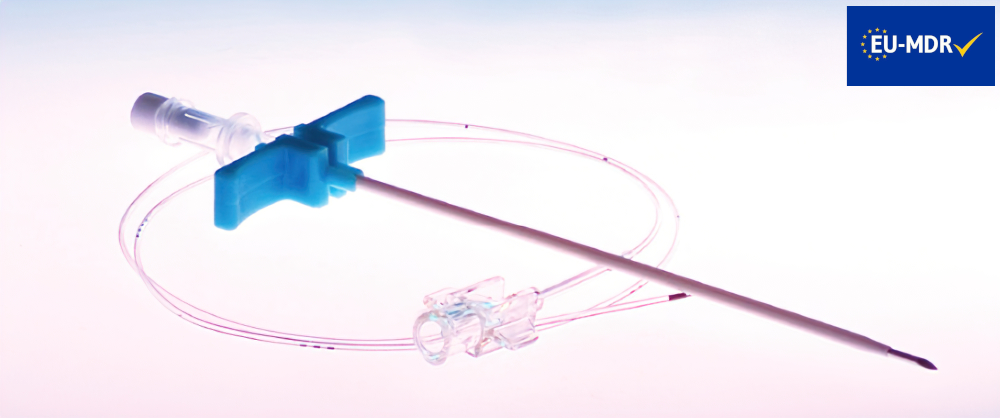
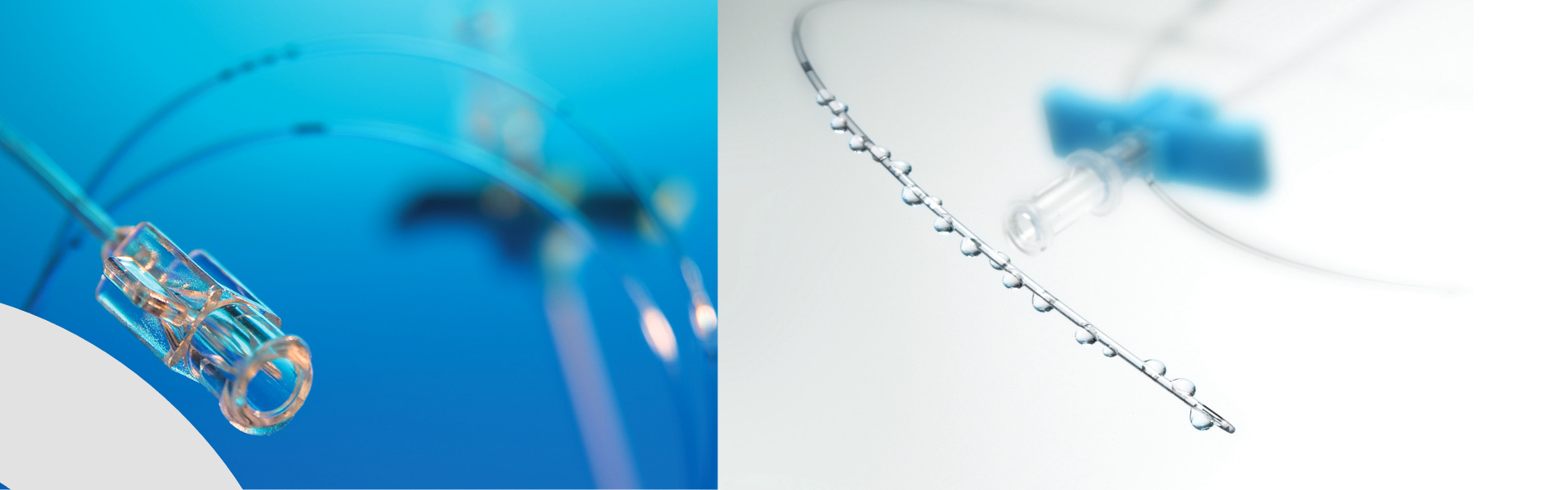
CONTINUOUS WOUND INFUSION
Continuous Wound Infusion (CWI) is a technique which uses a multi-holed catheter to deliver local anaesthetics or analgesics directly into the wound for postoperative pain relief.
It can be used as a single technique or as part of a multi-modal analgesic approach.
- Effective Postoperative Analgesia
The continuos wound infusion of local anaesthetics or analgesics has benn proven to provide effective postoperative analgesia for patients undegoing abdominaL, gynecological1, thoracic 2-3 and orthopedic surgeries4 – 7 as well as C section8 and hernia. 9 - Reduces Opioid Usage
Continuous wound infusion reduces the need for systemic opioids in the postoperative period.1 – 9 - Safe Technique
Continuous infusion of local anaesthetics or analgesics in the surgical wound for postoperative analgesia is a safe technique as it does not increase
the number of wound infections5 – 7 – 8, does not impair the wound healing process 5 – 7 – 8, and does not generate toxic levels of local anaesthetics in the patient’s plasma.1-5-7-8 - Reduces Hospitalisation
Some studies found that continuous wound infusion can reduce a patient’s lenght of stay in hospital.1 – 2 – 5 - Excellent Patient Satisfaction
Continuous wound infusion for postoperative analgesia provides excellent patient satisfaction. 5 – 6 – 8
- Radioopaque catheter with advanced design feature
to optimise uniform flow distribution - High tensile strength
indicating low risk of breakage10 - Convenient, easy to use system
with peel-away Introducer needle, dressing and catheter fixation - Range of 19 gauge catheters
to cover various incision lengths - Markings
to allow identification of multi-holed section, distance from the beginning of the multi-holed section and catheter integrity - Preconnected hub and hub sleeve
minimize the risk of disconnection or kinking after removal
CATHETERS FOR CONTINUOUS WOUND INFUSION
lenght |
lenght |
||
Catheter 2.5 |
|||
Catheter 7.5 |
|||
Catheter 15 |
|||
Catheter 22.5 |
|||
Catheter 30 |
REFERENCES
1. Beaussier M, El’ayoubi H, Schiffer E, Rollin M, Parc Y, Mazoit JX, Azizi L, Gervaz P, Rohr S, Biermann C, Lienhart A, Eledjam JJ. Continuous preperitoneal
infusion of ropivacaine provides effective analgesia and accelerates recovery after colorectal surgery: a randomized, double-blind, placebo-controlled study.
Anesthesiology. 2007 Sep;107(3):461-468.
2. Dowling R, Thielmeier K, Ghaly A, Barber D, Boice T, Dine A. Improved pain control after cardiac surgery: results of a randomized, double-blind, clinical trial.
J. Thorac. Cardiovasc. Surg. 2003 Nov;126(5):1271-8.
3. Karakaya D, Baris S, Ozkan F, Demircan S, Gok U, Ustun E, et al. Analgesic effects of interpleural bupivacaine with fentanyl for post-thoracotomy pain.
J Cardiothorac Vasc Anesth 2004 Aug;18(4):461-5.
4. Axelsson K, Nordenson U, Johanzon E, Rawal N, Ekback G, Lidegran G, et al. Patient-controlled regional analgesia (PCRA) with ropivacaine after arthro-
scopic subacromial decompression. Acta Anaesthesiol Scand 2003 Sep;47(8):993-1000.
5. Bianconi M, Ferraro L, Ricci R, Zanoli G, Antonelli T, Giulia B, et al. The pharmacokinetics and efficacy of ropivacaine continuous wound instillation after spine
fusion surgery. Anesth Analg 2004 Jan;98(1):166-72 table.
6. Blumenthal S, Dullenkopf A, Rentsch K, Borgeat A. Continuous infusion of ropivacaine for pain relief after iliac crest bone grafting for shoulder surgery.
Anesthesiology 2005 Feb;102(2):392-7.
7. Gottschalk A, Burmeister MA, Radtke P, Krieg M, Farokhzad F, Kreissl S, et al. Continuous wound infiltration with ropivacaine reduces pain and analgesic
requirement after shoulder surgery. Anesth Analg 2003 Oct;97(4):1086-91, table.
8. Fredman B, Shapiro A, Zohar E, Feldman E, Shorer S, Rawal N, et al. The analgesic efficacy of patientcontrolled ropivacaine instillation after Cesarean
delivery. Anesth Analg 2000 Dec;91(6):1436-40.
9. LeBlanc KA, Bellanger D, Rhynes VK, Hausmann M. Evaluation of continuous infusion of 0.5% bupivacaine by elastomeric pump for postoperative pain
management after open inguinal hernia repair. J Am Coll Surg 2005 Feb;200(2):198-202.
10. D. Thiveaud, V. Demazières, J. Lafont. Comparison of the performance of four elastomeric devices. EJHP 2005; P.2:56-6.